April 18, 2024
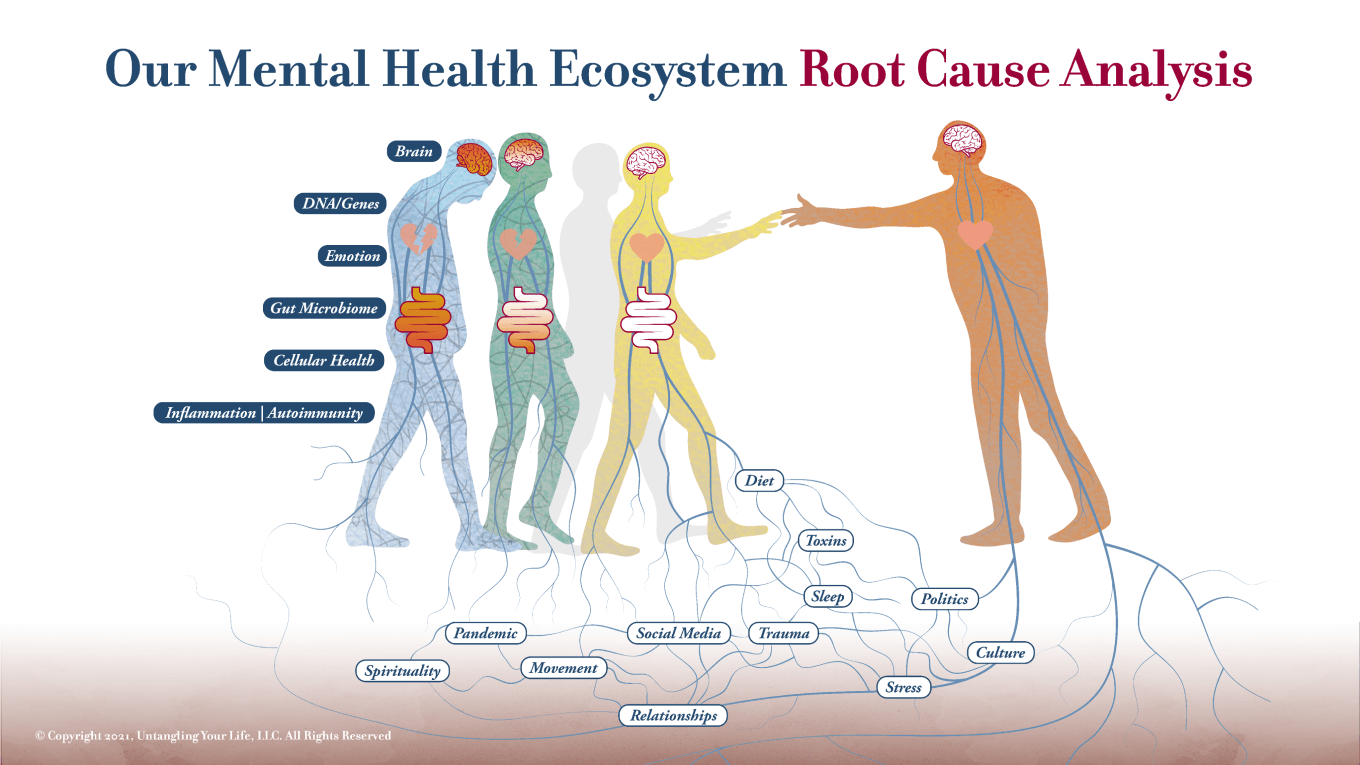
Unraveling the Mysteries of Resistant Anxiety and Depression: A Root Cause Psychiatry Success Story
Struggling with treatment-resistant anxiety or depression? Potomac Psychiatry offers hope. Explore our root cause approach that considers genetics, biochemistry, and more.
READ MORE